NEWS AND INFORMATION
FAQ
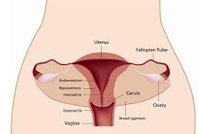
Even though cervical cancer rates have gone down in the last few decades, every woman needs to play a role in preventing cervical cancer and staying healthy. Regular check-ups, routine pap testing, and HPV testing when recommended, are key components in the fight against cervical cancer.

It is unlikely that you would be able to tell on your own. Precancerous cells and early cervical cancer usually don’t cause symptoms. That’s why routine pap testing is suggested for early detection and treatment. If you are experiencing unusual bleeding, pelvic pain, or urinary pain, you should speak with your doctor. The surest way to catch cervical cancer early is with regular screening and HPV testing when recommended.
Human papillomavirus (HPV) is a group of over 100 virus types that are transmitted by skin-to-skin contact. About 30-40 of these HPV strains are transmitted through sexual contact. About 80% of sexually active women have contracted at least one strain of genital HPV by age 50. Most HPV strains are harmless and clear on their own over time. However a few "high-risk" strains that may persist are associated with cervical cancer.
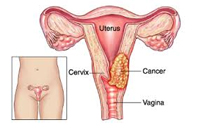
Not necessarily. The vast majority of women with an HPV infection never get cervical cancer. About 90% of HPV infections will clear on their own in two years.2.
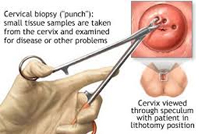
The cervical cancer screening test (pap test) involves collecting cells from the cervix and viewing them under a microscope to determine if they are precancerous or cancerous.
Since its introduction, cervical cancer deaths have declined by over 70%. Moreover, the advent of the liquid based cytology test alternative has contributed to an additional 28% decline in invasive cervical cancers in the United States.
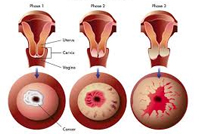
Yes. In many cases, cervical cancer does not cause symptoms until it is advanced. Regular cervical cancer screenings and HPV tests is the best way to aid in early detection.
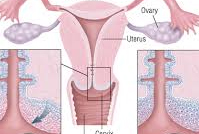
Over 90% of pap tests results come back as normal. In the event that your pap test comes back as abnormal, your doctor will recommend appropriate follow-up and possible treatment if necessary. Remember, when caught early, nearly all cervical cancers are treatable. The cervical cancer screening and HPV test when recommended, is the best method to aid in early detection.
Over 90% of pap tests results come back as normal. In the event that your pap test comes back as abnormal, your doctor will recommend appropriate follow-up and possible treatment if necessary. Remember, when caught early, nearly all cervical cancers are treatable. The cervical cancer screening and HPV test when recommended, is the best method to aid in early detection.
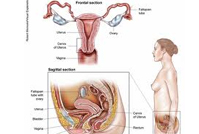
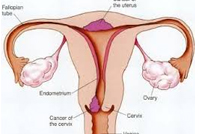
Cervical cancer affects mostly women over the age of 30. It is believed that cervical cancer is caused by a virus called human papillomavirus or HPV. The disease can be contracted through sexual contact with someone who has it
While there are different types of the HPV virus, not all types of HPV cause cervical cancer. Some of them cause genital warts, but other types may not show any symptoms.
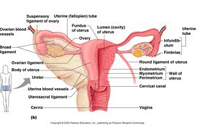
Gravely, the disease kills more women in India than any other countries in the world. Cervical cancer affects approximately 132,000 Indian women annually, of which an astounding 72,000 die, according to the Cervical Cancer-Free Coalition.
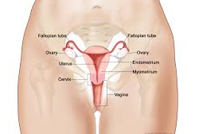
Signs and symptoms of cervical cancer may include - vaginal bleeding during sex, pelvic pain or pain during intercourse, change in menstrual cycle, bleeding in-between periods, post-menopausal bleeding, vaginal discharge tinged with blood that may have a foul odour.
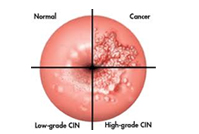
Treating cervical cancer is more likely to be successful if detected in its earliest stages. The American Cancer Society advises that all women should begin cervical cancer screening at age 21. It recommends that women aged 21 to 29, should have a Pap test every three years. Women who are age 30 or older should have a Pap test combined with an HPV test every five years till age 65 or just a Pap test every three years.
According to the Society, though the Pap smear is not foolproof in screening, it has been “more successful than any other test in preventing a cancer”. The Pap smear is available in several laboratories in Indian cities nowadays.
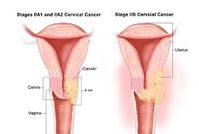
Treatment differs depending on stage of cancer and other health problems you may have. Treatment choices may include:
Surgery- Surgery is performed to remove the uterus (hysterectomy) in the early stages of cervical cancer
A simple hysterectomy is a surgical process to remove the cervix and the uterus.
A radical hysterectomy involves surgical removal of the cervix, uterus, part of the vagina and lymph nodes in the area
If you have a hysterectomy, you won’t become pregnant. But, hysterectomy isn’t always needed if cancer is detected very early.
Radiation- In this therapy, high dose of X-rays is used to destroy cancer cells and shrink tumours. It is a standard treatment for many types of cancer and may be used in combination with surgery, chemotherapy, or hormonal therapy.
Chemotherapy- It is the use of drugs/medicine to kill cancer cells. Certain chemotherapy drugs may lead to infertility as well as cause early menopause in premenopausal women.

You can reduce your risk of getting cervical cancer by following the tips below
- 1. Have regular Pap test screening
- 2. Get HPV vaccine
- 3. Do not smoke or if you do then quit smoking
- 4. Avoid having multiple sexual partners
- 5. Use condoms
- 6. Avoid all intimate sexual contact with anyone who has symptoms of STIs (sexually transmitted infections).

American Cancer Society. Guideline for Human Papillomavirus (HPV) Vaccine Use to Prevent Cervical Cancer and Its Precursors. Available here: caonline.amcancersoc.org.
Rodriguez, et al. Rapid clearance of human papillomavirus and implications for clinical focus on persistent infections. J Natl Cancer Inst. 2008;100:513-17.